The article that set me off on this rant—the proverbial straw that broke Lisa’s back– was the one that concluded like this: “Shawarma is the ultimate treatment for depression. No further studies are required to assess its efficacy anymore.” The article was on PubMed after having been published in Neuropsychology International. FYI, Shawarma is not a pharmaceutical agent. It’s that meat you see roasting on a spinning spit at Middle Eastern restaurants. I. Am. Not. Kidding.
 I know a lot of you come here for the funny, but today I’m not feeling funny at all, and the story about how Middle Eastern lunch meat could cure depression did not make me laugh. Granted, it wasn’t meant to, as it was published as a serious study, god help us all. But lately I have been thinking a lot about how this one aspect of the U.S. health system – mental healthcare — could not be further from good enough, and how much sadness and fear and lost lives this causes. Sorry to be Debbie Downer guys, but I just can’t laugh about it. Here’s why:
I know a lot of you come here for the funny, but today I’m not feeling funny at all, and the story about how Middle Eastern lunch meat could cure depression did not make me laugh. Granted, it wasn’t meant to, as it was published as a serious study, god help us all. But lately I have been thinking a lot about how this one aspect of the U.S. health system – mental healthcare — could not be further from good enough, and how much sadness and fear and lost lives this causes. Sorry to be Debbie Downer guys, but I just can’t laugh about it. Here’s why:
A few weeks back the Centers for Disease Control issued a report noting that, once again, life expectancy is dropping in the United States. Most upsetting is why life spans are shortening: mental health and substance abuse issues. This is a travesty.
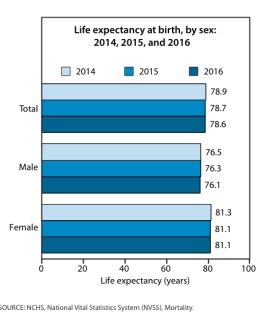
Specifically, as a story in Politico notes, “Americans who were born in 2017 are expected to live 78.6 years, a decrease of 0.1 from 2016. Suicide rates went up 3.7 percent in one year and 33 percent since 1999.” And “And more than 70,000 people died of a drug overdose in 2017, the highest number on record and 9.6 percent more than the previous year, according to the final mortality data. Overdose deaths involving fentanyl and certain other synthetic opioids increased 45 percent.”
 In the Politico story, Bob Anderson, chief of the Mortality Statistics Branch at the CDC’s National Center for Health Statistics, said, “We’re a developed nation with vast resources. There’s no reason we should be seeing life expectancy drop, this shouldn’t be happening.” Full story here.
In the Politico story, Bob Anderson, chief of the Mortality Statistics Branch at the CDC’s National Center for Health Statistics, said, “We’re a developed nation with vast resources. There’s no reason we should be seeing life expectancy drop, this shouldn’t be happening.” Full story here.
Since God was a child, we as a nation have failed to address head on the significant need for mental health and substance abuse treatment. We have been taught to be embarrassed to ask for it when we need it and quick to judge others who use it. And yet it is estimated that more than 20% of people could use some form of mental health care at some time in their lives and about 20 million suffer from substance abuse at any given time. I think these numbers are probably grossly underestimated.
I am often more surprised than I ought to be by the mental health tragedies I hear about from people who otherwise appear fully functional at work. Whether it’s their own challenge or that of a family member or other loved one, it’s so unusual to hear it openly spoken about, much less fully addressed. For one interesting example of this, listen to the recent Tech Tonics podcast featuring Sarah Iselin, a highly accomplished healthcare executive who suffered the loss of the love of her life to suicide while at the same time helping her son through a very difficult mental health challenge. And yet if you know Sarah or met her, you would think all is rosy and well – her resilience is remarkable. But it is worth remembering how many people live stories just like this; we rarely hear them out in the open, afraid as we are of being judged somehow broken, weird, off. Yet the number of people with mental health or substance abuse challenges outnumber those with high cholesterol or diabetes and we don’t shun or deny treatment to those with that diagnosis. Time to cut this crap out and take action.
What the hell is wrong with us that we can’t just recognize that conditions like depression and anxiety are normal and widespread, and that more serious conditions like bipolar disorder and schizophrenia are biological diseases that need to be treated just as cardiovascular disease or diabetes need to be treated – as chronic conditions, usually manageable with known therapies—so people can just live their lives. Why can’t we openly discuss these as we would our broken knee or diabetes or migraines or high cholesterol so we can help each other through the tough times? It’s getting better, but we are nowhere close. I am particularly perturbed by the suffering I have observed and read about among adolescents and young adults – not only are they under-treated, finding any professional who can actually help them is damn near impossible.
 Substance abuse, an entirely complex matter, has been with us from time immemorial, but the rise in opioid-related deaths is new and terrifying and infuriating. I’m glad we are seeing significant action to address these conditions and even some successes, like in Dayton, OH, where deaths from opioid use have dropped 50% as a result of a concerted and coordinated community effort. But the overall deaths are still going up and many of the treatment programs range from ineffective to awful. As a nation, we simply have to do better to help our fellow humans. Note that one day this could well be you if, God forbid, you break a hip or something that requires pain management. I have a nephew that started off with opioids and now he is so far gone with heroin we don’t know if he can ever come back. It is tragic to watch this once-promising and beautiful life turn into something so ugly and so lost.
Substance abuse, an entirely complex matter, has been with us from time immemorial, but the rise in opioid-related deaths is new and terrifying and infuriating. I’m glad we are seeing significant action to address these conditions and even some successes, like in Dayton, OH, where deaths from opioid use have dropped 50% as a result of a concerted and coordinated community effort. But the overall deaths are still going up and many of the treatment programs range from ineffective to awful. As a nation, we simply have to do better to help our fellow humans. Note that one day this could well be you if, God forbid, you break a hip or something that requires pain management. I have a nephew that started off with opioids and now he is so far gone with heroin we don’t know if he can ever come back. It is tragic to watch this once-promising and beautiful life turn into something so ugly and so lost.
Perhaps there is some help on the horizon. I am thrilled to see a plethora of new interest in behavioral health startup companies and new models that integrate access to mental health care with primary care. When, in 1998, I left the behavioral health company where I worked for nine years to join the venture world, I must have gone nearly 15 years without seeing any significant attempt to address the challenge. But lately, and especially in the last 5 years, there has been a rise in the number of companies with mental health and substance abuse care as a focus. The challenge is that virtually none of them have gotten to any kind of scale – most have struggled to get to $10mm in revenue, much less national scope. Another challenge is that not all of them take an evidence-based approach, and that is wrong. Don’t be out there making claims about how you can help people unless you can prove it.
We do, of course, have the big mental health and substance abuse program behemoths like Magellan (acquirer of my prior company in this area) and Beacon Health Options; but, with some exceptions, these are not companies primarily focused on delivering convenient access, financially affordable care or helping the average person find a really good match between patient and provider. Innovation is essential and thankfully we are beginning to see some.

Over the last year I have heard about companies taking head-on the challenge of predicting and preventing suicide, thank goodness (suicide make a big public appearance this year, offering up Kate Spade and Anthony Bourdain as celebrity spokespeople, among so many others). We have seen the rise of telemedicine for behavioral health to help overcome access issues. We have seen numerous Cognitive Behavioral Therapy (CBT) companies emerge to bring actionable means of treatment to larger segments of the population. But it is still way too hard to find the right therapist or treating clinician when you need one – it is too much of a crap shoot in a situation where quality really matters. And for many, the cost of treatment can be so far out of reach as to be unobtainable – I recently helped someone find a therapist and virtually all of those deemed “best” did not take insurance and charged well over $150 per hour. If you are not employed by a company or covered under a government health plan with generous benefits for mental health, it is really hard to find your way to care if you are even willing to admit you need it and/or ask for help. We need to put this stuff right out in the open and address it with new models.
I was very excited to see Walmart recently announce that, through a joint program with Beacon, they are opening their first retail mental health clinic in a Walmart store in Texas. I think that is a huge step in the right direction, not just in terms of accessibility, but in terms of addressing stigma. If treatment is normalized so it is just like going to the store for an eye exam, perhaps the people who need care can more readily get it. I have been very impressed by the work being done at HopeLabs for adolescents and teens and very intrigued by what has been achieved by Pear Therapeutics and others trying to tackle the opioid crisis as well as serious mental health conditions (Pear recently announced a product focused on schizophrenia care). Innovative companies like Freespira and even Verizon are working to address PTSD (Verizon recently donated 70,000 mobile lines to the VA to facilitate telebehavioral health for PTSD), an epidemic that must be addressed if we are going to truly honor our nation’s veterans. Telecare, a company that works largely with public entities to address the serious mental health and substance abuse conditions of under-served populations, has just announced some new approaches to substance abuse care that have great promise. There are many great people and companies I know who have dedicated their life to making major improvements in the lives of mental health patients and they are heroes who need more glory.
Last year I had the notable experience of being hosted at The Meeting Place by Shannon Jaccard, a friend and classmate in my Aspen Institute Fellowship and CEO of Ballast Health. The center, filled with people who have serious mental health issues, was wonderful, collegial, and a place for real peer support. It also helps them get jobs and find apartments and live regular lives. I’m sure some of our fellowship class were nervous and somewhat afraid about spending a morning there. But being there was joyful. Personally, I joined a table of people who were cutting out paper leaves for decorating their center Thanksgiving party and had a pretty damned good time. All the while, the members of the center talked openly about their hospitalizations, family challenges and hopes for the future. It was a very moving and warm experience and not scary at all. It was heartwarming and full of hope that people with serious challenges could find a good place in the social fabric to help them live their best lives.
I was also really delighted to see Cisco CEO Chuck Robbins write to all of his employees about the importance of mental health, particularly in the wake of some high-profile suicides and his heightened awareness of the needs of members of his own family. When you see successful people acknowledge that everything is not always hunky dory, that they too need help, you make it easier for everyone else. Similarly, Kate Spade Corp, an organization that knows first-hand the terrible impact of suicide, just announced it is donating $1 million to mental health organizations. Good on them. They could try to brush it under the rug and change their branding, but they haven’t. And for the holidays, Marc and Lynne Benioff, he of Salesforce fame, have recently donated $15 million to improve pediatric mental health in Oakland at the UCSF/Oakland Children’s Hospitals that bear his name. This generosity is to be applauded, and it is great to see money going where it is truly needed and mainstream leaders taking a stand.
The holiday time is incredibly intense for people who are stressed, depressed or otherwise challenged by mental health and substance abuse issues. I remember dreading the holidays because it made my mother, who suffered from both, particularly agitated and difficult. And yet everyone always just assumed all was well at home for me. I knew how to make it look like that, having learned over many years how to put up that front. And yet the truth was much darker. Few of my friends knew this and it made it hard to answer all those questions like, “you must be excited to see your family?!” Uh. Sort of. It’s complicated. That was my usual answer when I was being “transparent.” It took me years to realize that I would be better off by talking openly about it.
So, my ask of you is this: for the next few weeks, rather than judge people who seem angry, sad, cranky or otherwise disconnected for being unpleasant or unpredictable, think about how there may be so much more to the story than just a bad mood. This time of year, which is “SUPPOSED TO BE” all about joyous family reconnections, happy times, and other often unattainable expectations by some, remember that not everyone is feeling the love. Do your part to help people in need by cutting them a break, recognizing that they may be hurting and lending a helping hand if you can. If you’re giving money, consider NAMI or other charities that help people with mental health challenges. Hug a college kid who is having a rough time with their life transitions (20% of them are struggling with these issues). Be inclusive of friends who aren’t lucky enough to have families that function or friends in the area. In other words, just be open to the possibility and joy of helping someone through a particularly tough time. Don’t be afraid, by active. Make a difference and ask people if they are ok when they don’t seem ok. Be aware. Be a friend. Be kind.
And if you are the one who needs some help, please ask for it. We need you! Be brave and open your hearts and minds to available help; let people know what they can do and that you need someone to lean on. People are often willing to help when asked and there are resources out there for those who feel scared, alone, and unable to cope on their own. Here are some links to resources should you need them:
National Institute of Mental Health
And here are a few examples of telemedicine providers who specialize in behavioral health and that people can access directly on their own:
I wish you a calm holiday season. Beware of false shawarma prophets.



Lisa – Thank you for writing about this topic. It is so incredibly important that we find ways as a system to rejuvenate our approach to behavioral health. The holidays can be some of the toughest times for people experiencing hardships in this area, and we are not doing enough to combat the challenges (let alone make treatment accessible). I am glad to see this changing – albeit slowly.
At Kellogg’s Healthcare Conference this year, we have a great panel between a startup CEO and a government official talking about how to fight the opioid crisis: https://www.kelloggbhc.com/opioid-crisis/. I am very excited to listen!
Bravo Lisa!
Wish more healthcare thoughtleaders had your insights and initiative to change the status quo.
Thank you Cynthia. L
Thank you.
🙂
Lisa,
Thank you for this article and even though I love your humor, I appreciate you not joking about this subject. I have suffered from depression and know what it can be like. I also have had issues with substance abuse (28+ years ago). You are right, very little has been done by our government or corporations. It is good that we ae seeing more articles, publicity, action by some companies, etc.. However, as you point out we need so much more, especially making mental health and effective substance abuse programs economical for all.
John, thanks for sharing your story. Yes, much needs to be done. I’m encouraged by the activity and hoping for actual results. Lisa
Lisa-
Powerfully and courageously written- what sticks out to me is that 1) commercializing the holidays to be a time of joy and celebration just makes life tough on people who suffer from any spectrum of mental health issues or simply sadness, 2) stigma, yes there is still a stigma about many aspects of mental health and substance abuse so the more mainstream we can make this as any other condition the better, and 3) I celebrate my Dad’s life this time of year as I lost him when I was way too young on 12/29 and only learned to accept that loss by talking about it which brings me to 4) writing, talking and getting the word out will make everything better when it comes to having a healthy mental outlook and 5) we need more business innovation in this field to make a difference.
Thanks, Anne, for sharing your own personal thoughts. Lisa
Testify sistah sistah
Holla! L
Lisa, thank you for speaking out about this incredibly important issue. Access to mental health services has been as passion of mine for many years and then we lost my 24-year-old nephew to bipolar disorder and substance abuse just over a year ago, making the cause deeply personal.
One of the realities we must directly address is the chasm between need for mental health services and the available pool of professionals (even without the complicating issue of payment impeding access). There simply will never be enough professionals to meet the demand for care. The innovative start-ups you mentioned are critical to closing the chasm. Digitally enabled, clinically curated, self-care and peer care are proving to be very effective. Companies like SilverCloud and Big White Wall (both of which began in the UK) are proving that on-line cognitive behavioral therapy, clinically curated peer support and other on-line services can meet the need while also reducing the amount of live talk-therapy (whether in-person or virtual) required for improved health. Let’s work together to help the innovators with a strong evidence base scale. And, help “traditional” professionals embrace new modalities, incorporate them into their care plans and refer people to these new options to support adoption.
Frances, you and I are sympatico here! Lisa
Lisa, you are the voice of “we are better than this”. Thank you for the sensible advice, written in a way that displays your full passion. One of the many things I love about you.
As we trade “presents” for “presence”, let’s make this season about meaningful conversions and shining the light of love. Be aware. Be a friend. Be kind.
Thanks Maureen! Take care, miss you! Lisa
Thanks much for this Lisa. Incredibly well said. You are brave, funny, articulate, well informed and, as usual, brutally honest. You are one of the people that is making a difference, and will help change these horrible stats. And you continue to motivate and energize others to be part of the cause. Wishing you and your loved ones peace and happiness this holiday season. Rob
Rob, thank you so much for those kind words. Wishing you a wonderful holiday too. Be well, Lisa